All Posts
-
Best gastroenterologist in Khulna.
Are you looking for the best gastroenterologist in Khulna to treat your digestive health issues? Whether you’re dealing with chronic acidity, liver problems, ulcer, or other gastrointestinal concerns, finding the right gastroenterologist in Khulna is crucial for proper diagnosis and treatment.
In this blog, we’ll guide you through the top-rated specialists in Khulna who are experienced in managing all kinds of stomach, liver, and intestinal problems. Read on to find out where you can get the best care from the best gastroenterologist in Khulna.

Assistant Professor Dr. Shahidul Hasan Shahin
Gastroenterologist
MBBS, MD (Gastroenterology), BSMMU (Dhaka), Gastroenterology, Pancreas and Liver Medicine Specialist, Endoscopy and Colonoscopy Specialist - Khulna Medical College Hospital.
Chamber Address: 37, K D A Avenue, Khulna-9100.
View doctor profile Click here
For serial call 01740-486123 (10:00 AM to 07:00 PM, Excluding Fridays)

Assistant Professor Dr. Birendranath Saha
Gastroenterologist
MBBS, BCS (Health), MD (Gastroenterology). Specialist in Gastroenterology, Digestive System, Pancreas, and Liver Diseases. Assistant Professor - Shaheed Tajuddin Medical College.
Chamber Address: 37, K D A Avenue, Khulna-9100.
View doctor profile Click here
For serial call 01740-486123 (10:00 AM to 07:00 PM, Excluding Fridays)

Dr. Marina Rahman
Gastroenterologist
MBBS, BCS (Health), MD (Hepatology), Interventional Hepatologist (Department of Hepatology) - Khulna Medical College Hospital, Khulna.
Chamber Address: 37, K D A Avenue, Khulna-9100.
View doctor profile Click here
For serial call 01740-486123 (10:00 AM to 07:00 PM, Excluding Fridays)

Dr. Sheikh Md. Rezwan
Gastroenterologist
MBBS, FCGP, MSc Gastroenterology (CSI) - Consultant, Citizen Lab Medicine, Liver, Pancreas & Digestive System Specialist.
Chamber Address: Islam Tower, 22 KDA Avenue, Moylapota, Khulna.
View doctor profile Click here
For serial call 01740-486123 (10:00 AM to 07:00 PM, Excluding Fridays)
Who Is a Gastroenterologist? – Everything You Need to Know
A gastroenterologist is a medical doctor who specializes in diagnosing and treating conditions related to the digestive system. This includes the esophagus, stomach, intestines, liver, pancreas, and gallbladder. If you’ve ever experienced persistent stomach pain, acid reflux, constipation, or other digestive issues, a gastroenterologist is the specialist you need to consult.
What Does a Gastroenterologist Do?
Gastroenterologists focus on the function and diseases of the gastrointestinal (GI) tract. Their work includes:
-
Diagnosing and treating digestive disorders
-
Performing endoscopic procedures (like colonoscopy and endoscopy)
-
Managing chronic diseases like ulcerative colitis and Crohn's disease
-
Helping with liver conditions such as hepatitis and fatty liver
-
Treating gastroesophageal reflux disease (GERD) and ulcers
They are highly trained experts who understand the complex mechanisms of digestion, absorption, and waste elimination.
When Should You See a Gastroenterologist?
You should consider visiting a gastroenterologist if you experience:
-
Persistent abdominal pain or bloating
-
Chronic heartburn or acid reflux
-
Difficulty swallowing
-
Blood in your stool or black, tarry stools
-
Frequent constipation or diarrhea
-
Unexplained weight loss
-
Liver problems or abnormal liver function tests
Early diagnosis of digestive issues can prevent complications and improve your quality of life.
Common Procedures Performed by Gastroenterologists
Gastroenterologists use advanced diagnostic tools and procedures, including:
-
Endoscopy – to view the esophagus, stomach, and small intestine
-
Colonoscopy – to screen for colon cancer or check for polyps
-
ERCP (Endoscopic Retrograde Cholangiopancreatography) – to diagnose gallbladder and bile duct issues
-
Liver biopsy – to diagnose liver conditions
-
Capsule endoscopy – using a small camera pill to see inside the small intestine
These procedures help detect diseases early and ensure effective treatment.
How to Keep Your Digestive System Healthy?
While a gastroenterologist can treat your digestive issues, prevention is better than a cure. Follow these tips for a healthier gut:
-
Eat a fiber-rich diet (vegetables, fruits, whole grains)
-
Stay hydrated
-
Avoid overeating and junk food
-
Reduce stress
-
Limit alcohol and stop smoking
-
Don’t ignore unusual symptoms
FAQ about Gastroenterologists
1. What is a gastroenterologist?
A gastroenterologist is a medical doctor who specializes in diagnosing and treating conditions related to the digestive system, including the stomach, intestines, liver, pancreas, esophagus, and gallbladder.
2. When should I see a gastroenterologist?
You should see a gastroenterologist if you have persistent digestive symptoms such as abdominal pain, bloating, diarrhea, constipation, heartburn, rectal bleeding, or difficulty swallowing.
3. What procedures does a gastroenterologist perform?
Gastroenterologists perform diagnostic and therapeutic procedures such as endoscopy, colonoscopy, sigmoidoscopy, liver biopsy, and polyp removal, among others.
4. Do I need a referral to see a gastroenterologist?
In many cases, yes. Depending on your healthcare system or insurance policy, you might need a referral from your primary care physician before seeing a gastroenterologist.
5. What conditions does a gastroenterologist treat?
They treat a wide range of conditions, including acid reflux (GERD), peptic ulcers, irritable bowel syndrome (IBS), Crohn's disease, ulcerative colitis, hepatitis, pancreatitis, and colon cancer.
Final Thoughts
A gastroenterologist plays a vital role in maintaining your digestive health. From minor symptoms to serious conditions like colon cancer or liver disease, their expertise can help you get the right diagnosis and treatment. If you’re experiencing ongoing digestive issues, don’t delay — consult a qualified gastroenterologist and take the first step toward a healthier you.
- Category : Blogpage
- 2025-06-21
- Views : 1573
-
-
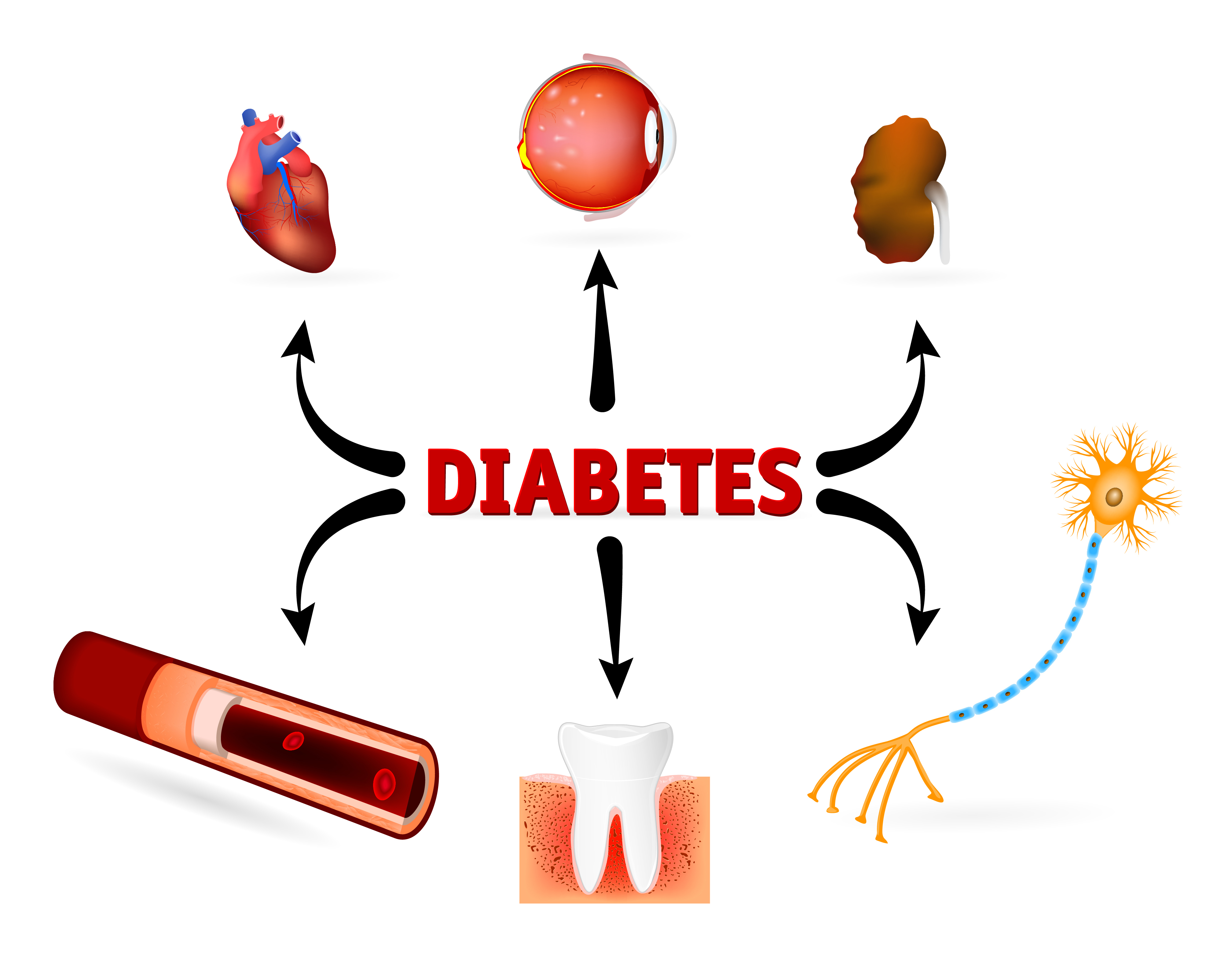
What is Diabetes Mellitus? A Complete Guide for Beginners
Diabetes mellitus is one of the most common and challenging chronic diseases in the world today. Affecting millions of people across all age groups, diabetes can lead to serious health complications if not managed properly. But what exactly is diabetes mellitus? What causes it, what are the types, symptoms, and treatments? In this blog post, we’ll explore everything you need to know about this condition and guide you on how to find the best diabetes doctor for treatment and support.
What is Diabetes Mellitus?
Diabetes mellitus is a chronic metabolic disorder in which the body is unable to properly regulate blood glucose (sugar) levels. This occurs either because the body doesn’t produce enough insulin or because the body’s cells do not respond properly to insulin.
What is Insulin?
Insulin is a hormone produced by the pancreas that allows cells to absorb glucose from the bloodstream to use as energy. Without proper insulin function, sugar builds up in the blood, leading to high blood sugar levels the hallmark of diabetes.
Types of Diabetes Mellitus
There are several types of diabetes, each with unique characteristics:
1. Type 1 Diabetes
- An autoimmune condition where the body attacks its own insulin-producing cells.
- Usually develops in childhood or adolescence.
- Patients must take daily insulin injections.
- Also known as insulin-dependent diabetes.
2. Type 2 Diabetes
- The most common form of diabetes.
- The body either doesn’t produce enough insulin or doesn’t use it effectively (insulin resistance).
- Often develops in adults over 40, but is increasingly seen in younger people.
- Linked to obesity, poor diet, and inactivity.
3. Gestational Diabetes
- Occurs during pregnancy.
- Usually temporary, but it increases the risk of developing type 2 diabetes later.
- It can affect the health of both mother and baby if not properly managed.
4. Prediabetes
- A condition where blood sugar levels are higher than normal but not yet high enough for a diabetes diagnosis.
- A warning sign that diabetes may develop without lifestyle changes.
Common Symptoms of Diabetes Mellitus
Recognizing the early signs of diabetes can lead to faster diagnosis and treatment. Common symptoms include:
- Frequent urination (especially at night)
- Excessive thirst
- Unexplained weight loss
- Increased hunger
- Fatigue
- Blurred vision
- Slow-healing wounds
- Tingling or numbness in hands or feet
- Frequent infections (skin, gum, urinary)
Some people with type 2 diabetes may not notice symptoms for years, making regular blood sugar tests important, especially for those with risk factors.
Causes and Risk Factors
Several factors contribute to the development of diabetes:
- Genetics: A Family history of diabetes increases risk.
- Obesity: Excess body fat, particularly around the abdomen, is strongly linked to type 2 diabetes.
- Physical inactivity: Lack of exercise contributes to insulin resistance.
- Unhealthy diet: High sugar and processed food intake raise blood sugar levels.
- Age: Risk increases after age 45.
- Other conditions: High blood pressure, high cholesterol, or PCOS may also raise the risk.
Complications of Diabetes Mellitus
If left unmanaged, diabetes can lead to serious health complications, including:
- Heart disease and stroke
- Kidney failure
- Nerve damage (neuropathy)
- Eye problems (diabetic retinopathy, blindness)
- Foot ulcers and amputations
- Sexual dysfunction
That’s why early diagnosis and long-term management are crucial.
Diagnosis of Diabetes
Diabetes is diagnosed through various blood tests, such as:
- Fasting Blood Sugar (FBS): Measures blood glucose after 8 hours of fasting.
- Oral Glucose Tolerance Test (OGTT): Measures the body’s response to sugar intake.
- Hemoglobin A1c Test: Reflects average blood sugar levels over the past 2-3 months.
Treatment and Management
There is no permanent cure for diabetes, but it can be effectively managed through:
1. Medications
- Type 1 Diabetes: Requires lifelong insulin therapy.
- Type 2 Diabetes: Managed with oral medications (like metformin), and sometimes insulin.
2. Dietary Control
- Eat balanced meals with whole grains, vegetables, lean proteins, and low sugar.
- Control portion sizes and avoid sugary drinks and processed foods.
3. Regular Exercise
- Helps control blood sugar, reduce weight, and improve heart health.
4. Blood Sugar Monitoring
- Self-monitoring helps patients adjust diet, exercise, and medications as needed.
5. Regular Checkups
- Routine visits with a dialectologist or endocrinologist are essential to monitor complications and adjust treatment plans.
If you’re living in Dhaka and searching for expert care, it’s wise to consult the best diabetes doctor in Dhaka for personalized treatment and long-term health monitoring.
Prevention Tips for Type 2 Diabetes
While type 1 diabetes is not preventable, type 2 diabetes can often be delayed or prevented with:
- Healthy eating habits
- Regular physical activity
- Weight loss (if overweight)
- Avoiding smoking and excessive alcohol
- Regular health checkups and blood sugar monitoring
Final Words
Diabetes mellitus is a serious condition, but with the right knowledge, lifestyle changes, and medical care, people can lead full and active lives. Understanding what diabetes is—and taking early steps to manage or prevent it—is key to avoiding long-term complications.
If you or a loved one is showing symptoms or has been diagnosed with diabetes, seek medical advice from the best diabetes doctor to get a tailored treatment plan and proper guidance.
- Category : Blogpage
- 2025-06-03
- Views : 476
-
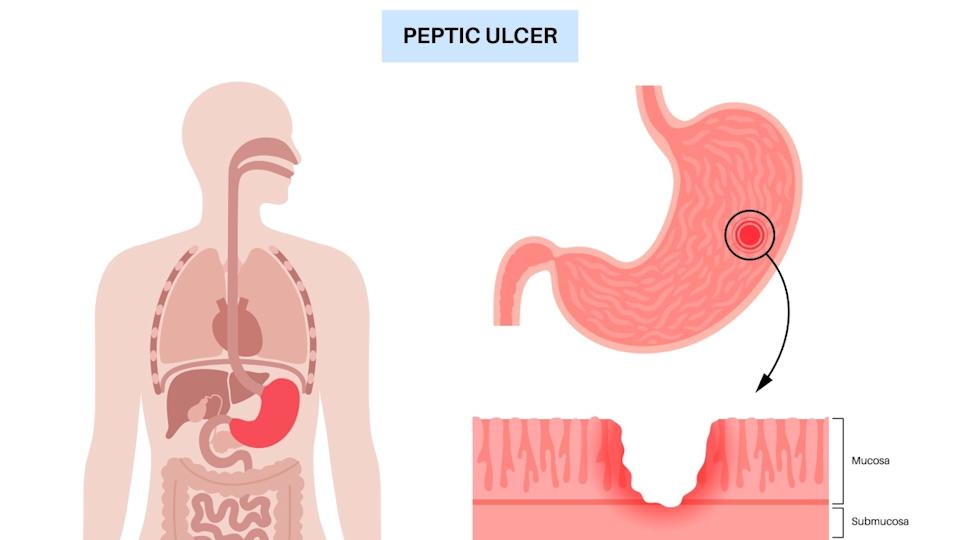
Peptic Ulcer Symptoms: What You Need to Know
A peptic ulcer is a sore that develops on the lining of the stomach, small intestine, or esophagus due to the erosion caused by stomach acid. This condition can lead to a variety of uncomfortable and sometimes serious symptoms. While some people may not experience noticeable signs at first, others might face persistent discomfort that should not be ignored.
In this blog post, we will cover everything you need to know about peptic ulcer symptoms, their causes, potential complications, and when to see a doctor. Whether you're experiencing digestive issues or just want to stay informed, this guide is for you.
What Is a Peptic Ulcer?
A peptic ulcer occurs when the protective mucous lining of the stomach or duodenum (the first part of the small intestine) becomes damaged, allowing acid to eat away at the tissues underneath. There are two main types of peptic ulcers:
- Gastric ulcers: Occur in the stomach lining.
- Duodenal ulcers: Occur in the upper part of the small intestine.
Causes of Peptic Ulcers
Several factors contribute to the development of peptic ulcers:
- Helicobacter pylori (H. pylori) infection – a common bacterial infection that damages the stomach lining.
- Long-term use of NSAIDs (nonsteroidal anti-inflammatory drugs) such as ibuprofen and aspirin.
- Excessive alcohol consumption
- Smoking
- Stress (although not a direct cause, it can worsen symptoms)
- Spicy foods may irritate existing ulcers.
Common Peptic Ulcer Symptoms
Symptoms can vary depending on the location and severity of the ulcer. Here are the most common signs:
1. Burning Stomach Pain
This is the hallmark symptom. The pain is usually felt between the breastbone and navel and often occurs:
- On an empty stomach
- At night
- Between meals
The pain may be temporarily relieved by eating or taking antacids but often returns.
2. Bloating
You may feel full quickly when eating or feel bloated for extended periods.
3. Nausea or Vomiting
Many people with peptic ulcers experience nausea. In severe cases, vomiting may occur, sometimes with blood (which appears red or like coffee grounds).
4. Loss of Appetite
Ongoing discomfort often reduces the desire to eat, leading to weight loss.
5. Weight Loss
Unintentional weight loss is a red flag, especially if it happens alongside other ulcer symptoms.
6. Dark or Tarry Stools
This can indicate internal bleeding and should be treated as a medical emergency.
7. Chest Pain
Some ulcers cause pain that mimics heartburn or even heart attack symptoms.
Silent Ulcers: No Symptoms
It’s important to note that some peptic ulcers cause no noticeable symptoms. These are called “silent ulcers” and are often discovered during endoscopy or after complications like bleeding.
When to See a Doctor
Seek medical attention if you have:
- Persistent or severe abdominal pain
- Blood in vomit or stools
- Difficulty eating or keeping food down
- Unexplained weight loss
These could be signs of a serious complication, such as perforation or internal bleeding.
Diagnosis of Peptic Ulcers
A healthcare provider may use the following tests to diagnose a peptic ulcer:
- Endoscopy: A camera is used to view the stomach and duodenum.
- H. pylori tests: Via breath, blood, stool, or biopsy during endoscopy.
- Barium swallow: X-ray imaging after drinking a contrast solution.
Early diagnosis can prevent complications and ensure effective treatment.
Treatment Options
1. Medications
- Antibiotics to kill H. pylori bacteria
- Proton pump inhibitors (PPIs) to reduce stomach acid
- H2-receptor blockers
- Antacids
- Cytoprotective agents to protect the stomach lining
2. Lifestyle Changes
- Avoid NSAIDs
- Quit smoking
- Limit alcohol
- Eat a balanced, non-irritating diet
3. Surgery (rare)
In cases of severe complications like perforation, obstruction, or non-healing ulcers, surgery may be required.
Complications of Untreated Peptic Ulcers
If left untreated, peptic ulcers can lead to:
- Internal bleeding
- Perforation (a hole in the stomach wall)
- Gastric outlet obstruction
- Increased risk of stomach cancer (especially with chronic H. pylori infection)
That’s why timely diagnosis and expert medical care are essential.
Consult the Best Gastroenterologist in Dhaka
If you're experiencing symptoms of a peptic ulcer, it's vital to get evaluated by a qualified specialist. A proper diagnosis and treatment plan can prevent complications and ensure long-term relief. If you're looking for expert care, consult the best gastroenterologist in Dhaka for accurate diagnosis, endoscopy services, and personalized treatment.
These specialists have extensive experience in managing complex gastrointestinal disorders, including peptic ulcers caused by H. pylori, medication, or lifestyle factors.
Final Thoughts
Peptic ulcers are a common but potentially serious condition that requires timely medical attention. The symptoms can range from mild discomfort to severe pain and bleeding. Recognizing the signs early and seeking treatment can significantly improve your health outcomes.
- Category : Blogpage
- 2025-06-03
- Views : 226
-
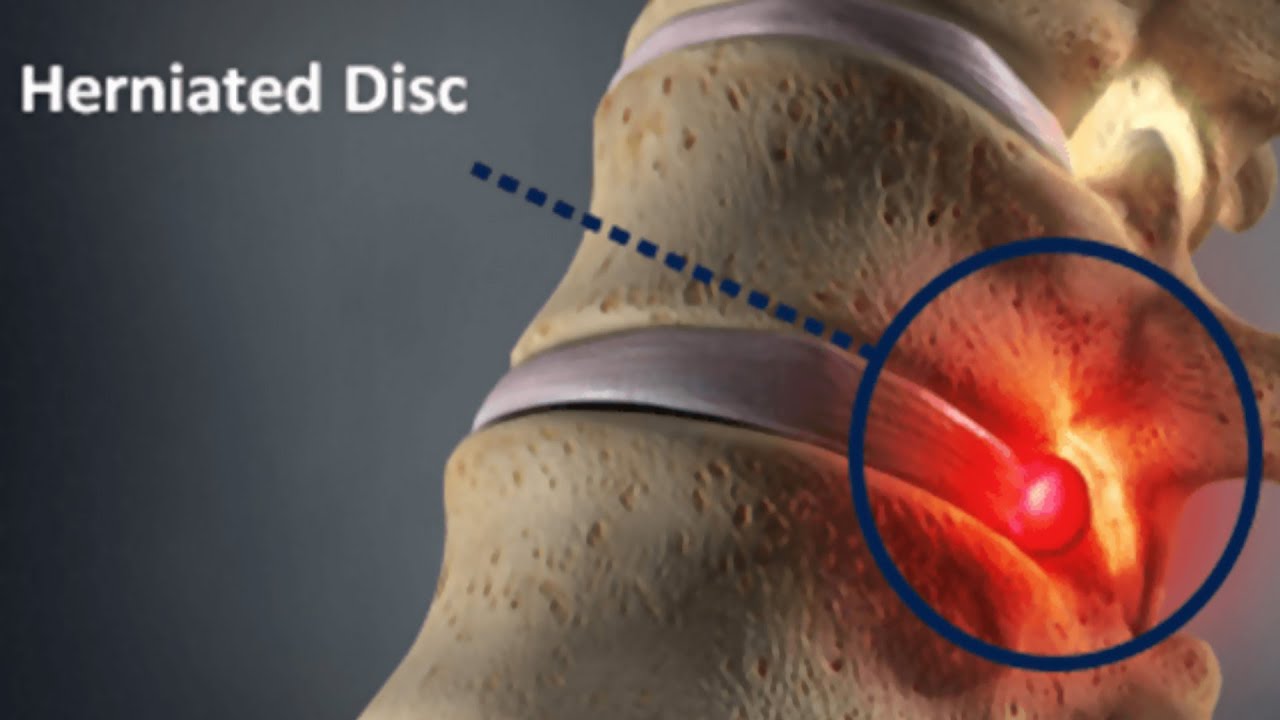
Herniated Disk Treatment: Symptoms, Diagnosis, and Options
A herniated disk, also known as a slipped or ruptured disk, is a common spinal condition that can cause pain, numbness, and weakness. It occurs when the soft inner gel of a spinal disk leaks out through a tear in the tougher exterior. This often leads to pressure on nearby nerves, resulting in discomfort that can range from mild to debilitating.
Understanding herniated disk treatment is essential for those seeking relief and hoping to regain a better quality of life. In this blog, we will explore the causes, symptoms, diagnosis, and the latest treatment options available for a herniated disk.
What Causes a Herniated Disk?
A herniated disk can be the result of several factors, including:
- Aging and disk degeneration: With age, spinal disks lose water content, making them less flexible and more prone to tearing or rupturing.
- Injury or trauma: Sudden strain or heavy lifting can cause a disk to herniate.
- Repetitive motions: Activities that involve twisting or turning the back repeatedly may contribute to disk herniation.
- Poor posture: Long-term poor posture can lead to excessive stress on the spine.
- Genetics: Some people inherit a predisposition to developing disk problems.
Common Symptoms of a Herniated Disk
The symptoms vary depending on the location of the herniated disk and whether it presses on a nerve. Common signs include:
- Pain in the lower back or neck
- Radiating pain to the arms or legs
- Numbness or tingling sensations
- Muscle weakness
- Difficulty moving or walking
Pain usually worsens with movement and may improve with rest. In severe cases, it may cause problems with bladder or bowel control, which requires emergency medical attention.
How is a Herniated Disk Diagnosed?
If you suspect a herniated disk, it’s important to consult a healthcare professional. A proper diagnosis usually involves:
- Medical history and physical examination
- Neurological exams to check muscle strength and reflexes
- Imaging tests:
- MRI (Magnetic Resonance Imaging): Most effective for viewing herniated disks
- CT scans
- X-rays
- Myelogram (in some cases)
These tests help determine the location and severity of the herniation, which is essential in choosing the most suitable treatment plan.
Non-Surgical Treatments for a Herniated Disk
In many cases, herniated disks can be managed without surgery. Non-surgical treatment options include:
1. Rest and Activity Modification
Short periods of rest followed by gentle movement can ease symptoms. Avoid heavy lifting and strenuous activities.
2. Medications
- Pain relievers (NSAIDs): Ibuprofen or naproxen to reduce inflammation and pain
- Muscle relaxants: To relieve spasms
- Corticosteroids: Either oral or injected to reduce nerve inflammation
3. Physical Therapy
A physical therapist can teach exercises to:
- Strengthen back and abdominal muscles
- Improve posture and flexibility
- Reduce pressure on the affected nerve
4. Epidural Steroid Injections
These injections are administered directly into the spine to reduce inflammation around the herniated disk and provide pain relief.
When is Surgery Needed?
Surgery is recommended when:
- Non-surgical treatments fail after 6–12 weeks
- There is significant weakness, numbness, or nerve damage
- The herniated disk is causing bowel or bladder dysfunction
The most common surgical procedures include:
1. Microdiscectomy
A minimally invasive surgery that removes the herniated portion of the disk, relieving pressure on the nerve.
2. Laminectomy
Removal of a portion of the vertebral bone (lamina) to create space and reduce nerve pressure.
3. Spinal Fusion
Sometimes needed to stabilize the spine after a disk is removed.
4. Artificial Disk Replacement
In some cases, the damaged disk is replaced with an artificial one to maintain mobility.
Recovery and Rehabilitation
Post-surgery recovery may take a few weeks to a few months. Most patients experience significant relief from symptoms. A tailored rehabilitation plan helps regain strength and flexibility. It’s crucial to follow the surgeon’s instructions and attend follow-up visits.
Finding the Right Specialist
For individuals suffering from severe herniated disk issues, especially those requiring surgical intervention, consulting a qualified spine specialist is crucial. If you're in Bangladesh, it’s essential to consult with the Best spine surgeon in Bangladesh to receive expert care and treatment.
These specialists are highly experienced in both conservative and surgical treatments, ensuring you receive a tailored approach to your condition.
Tips to Prevent Herniated Disks
- Maintain good posture
- Exercise regularly, focusing on core strength
- Use proper lifting techniques
- Avoid prolonged sitting or repetitive strain
- Maintain a healthy weight
Final Thoughts
A herniated disk can be a painful and disabling condition, but with the right treatment, most people can recover fully or experience significant relief. Whether through physical therapy or surgery, early diagnosis and appropriate treatment are key to preventing long-term complications.
If you're facing persistent back or neck pain, don’t ignore it. Consult a spine specialist today and explore your treatment options for a better, pain-free life.
- Category : Blogpage
- 2025-06-03
- Views : 85
-
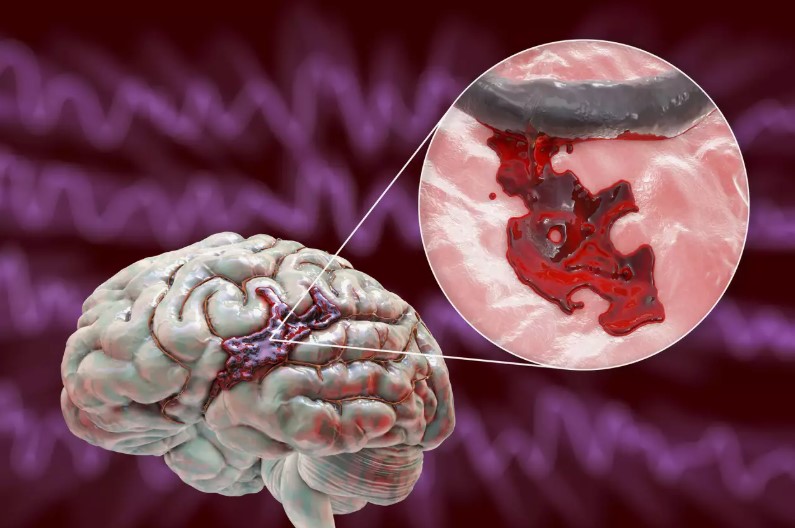
Brain Hemorrhage Symptoms: Early Warning Signs You Should Never Ignore
A brain hemorrhage, also known as an intracranial hemorrhage, is a type of stroke caused by bleeding in the brain. It is a life-threatening medical emergency that requires immediate attention. Understanding the symptoms of a brain hemorrhage can help save lives, especially when time is of the essence.
In this blog post, we’ll take an in-depth look at the symptoms, causes, risk, and factors.
What Is a Brain Hemorrhage?
A brain hemorrhage occurs when a blood vessel in the brain ruptures, causing blood to leak into the surrounding brain tissue. Leaked blood can increase pressure on the brain, damage brain cells, and restrict the oxygen supply. Trauma, high blood pressure, aneurysms, blood vessel abnormalities, or bleeding disorders can cause brain hemorrhages.
There are several types of brain hemorrhages, including:
- Intracerebral hemorrhage: Bleeding within the brain tissue.
- Subarachnoid hemorrhage: Bleeding in the space between the brain and the thin tissues covering the brain.
- Subdural and epidural hematomas: Bleeding between the skull and brain layers.
Common Brain Hemorrhage Symptoms
Recognizing the early signs of a brain hemorrhage is vital. The symptoms may vary depending on the location and severity of the bleeding, but the following are some of the most common:
1. Sudden and Severe Headache
One of the most classic symptoms of a brain hemorrhage is a sudden, intense headache. Patients often describe it as the worst headache of their life. This pain can be sharp, persistent, and may come on without warning.
2. Nausea and Vomiting
The increased pressure on the brain due to bleeding can cause nausea and vomiting, often accompanying a severe headache.
3. Weakness or Numbness
Bleeding in the brain can affect muscle control and sensation, often leading to sudden weakness or numbness, typically on one side of the body.
4. Loss of Consciousness
As the brain swells or becomes deprived of oxygen, a person may faint, lose consciousness, or fall into a coma.
5. Seizures
A brain hemorrhage can trigger abnormal electrical activity, resulting in seizures. These may include convulsions or moments of unresponsiveness.
6. Vision Problems
People may experience blurred or double vision, or even loss of vision in one or both eyes, depending on the part of the brain affected.
7. Difficulty Speaking or Understanding Speech
Speech can become slurred or incoherent, and the patient may struggle to form or understand words.
8. Difficulty Walking or Poor Coordination
The person may lose balance, have trouble walking, or appear unsteady.
9. Tingling Sensations
A sensation of pins and needles or tingling can be an early sign, especially if it occurs suddenly.
10. Confusion and Behavioral Changes
Brain function can be severely affected, leading to confusion, irritability, and sudden mood changes.
Causes and Risk Factors of Brain Hemorrhage
Brain hemorrhages can result from various causes, including:
- High blood pressure (hypertension) – the leading cause
- Head injury or trauma
- Aneurysms (weakened blood vessel walls)
- Arteriovenous malformations (AVMs)
- Blood clotting disorders
- Brain tumors
- Use of blood thinners or anticoagulants
- Substance abuse (especially cocaine or amphetamines)
When to Seek Immediate Medical Help
A brain hemorrhage is a medical emergency. If you or someone around you exhibits any of the symptoms mentioned above, do not delay—call emergency services immediately.
Quick diagnosis and treatment can significantly increase the chances of survival and reduce the risk of long-term brain damage.
Diagnosis and Treatment
Doctors typically use CT scans or MRIs to confirm a brain hemorrhage. Once diagnosed, treatment may involve:
- Medications to control blood pressure, seizures, or brain swelling
- Surgery to remove blood clots, relieve pressure, or repair damaged blood vessels
- Rehabilitation for regaining motor skills, speech, or cognitive function
The outcome depends on the size and location of the hemorrhage and how quickly the patient receives treatment.
Best Neurosurgeon in Bangladesh
If you or your loved one is at risk of brain hemorrhage or recovering from one, it is crucial to consult with an experienced specialist. Selecting the best neurosurgeon in Bangladesh can ensure accurate diagnosis, precise surgery, and effective rehabilitation planning. These experts are trained to handle complex brain conditions with advanced techniques and state-of-the-art technology.
Final Thoughts
A brain hemorrhage can be sudden and devastating. But early detection of symptoms like a severe headache, confusion, weakness, or loss of speech can be life-saving. Never ignore these signs time is brain.
- Category : Blogpage
- 2025-06-03
- Views : 686
-
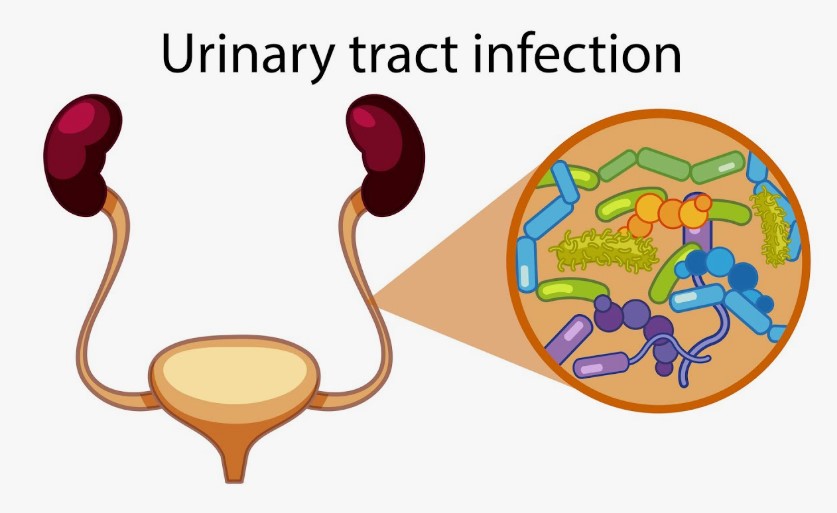
Urine Infection Symptoms: Causes, Signs, and When to See a Urologist
Urinary Tract Infections (UTIs), commonly known as urine infections, are a widespread health concern affecting millions of people globally each year. These infections can impact any part of the urinary system—including the kidneys, ureters, bladder, and urethra—but are most commonly found in the lower urinary tract (the bladder and urethra).
Although urine infections are usually not serious when treated early, they can lead to severe complications like kidney infections if ignored. This blog post explores urine infection symptoms, causes, risk factors, prevention tips, and when to consult a urologist
What Is a Urinary Tract Infection (UTI)?
A UTI is an infection caused by bacteria, most commonly Escherichia coli (E. coli), which normally lives in the intestines but can enter the urinary tract through the urethra. UTIs are more common in women due to their shorter urethra, which makes it easier for bacteria to reach the bladder.
Common Causes of Urine Infection
- Bacterial Contamination: Most commonly from E. coli.
- Poor Hygiene: Wiping from back to front can introduce bacteria.
- Holding Urine: Delaying urination can allow bacteria to multiply.
- Sexual Activity: Increases the risk of bacterial transfer.
- Use of Catheters: Can introduce bacteria into the bladder.
- Weakened Immune System: Reduces the body’s ability to fight off infections.
Who Is at Risk?
While anyone can get a urine infection, some groups are more vulnerable:
- Women, especially those who are sexually active or pregnant
- Older adults
- People with diabetes
- Individuals with kidney stones
- Those with a suppressed immune system
- Patients with urinary catheters
Urine Infection Symptoms
Urine infection symptoms can vary depending on the part of the urinary tract affected. Here’s a breakdown:
1. Lower UTI (Bladder and Urethra)
- Burning Sensation While Urinating: A classic symptom of bladder infection.
- Frequent Urge to Urinate: Even when little urine is passed.
- Cloudy or Bloody Urine: May appear pink, red, or brownish.
- Strong-Smelling Urine: Foul or unusual odor.
- Pelvic Pain: Especially in women, usually centered around the pubic bone.
- Discomfort or Pressure in the Lower Abdomen
2. Upper UTI (Kidneys)
- Fever and Chills
- Nausea or Vomiting
- Pain in the Flanks or Back
- Fatigue
- Confusion (especially in elderly patients)
Important: A kidney infection (pyelonephritis) is a serious condition and requires immediate medical attention.
UTI Symptoms in Men
Although less common, men can also suffer from UTIs. Symptoms include:
- Burning or pain while urinating
- Frequent urination
- Discharge from the penis
- Pain in the rectum, lower abdomen, or back
Urine Infection in Children
In children, symptoms may include:
- Bedwetting
- Fever without a clear cause
- Irritability
- Poor feeding (in infants)
UTIs in children must be addressed promptly to avoid complications.
When to See a Urologist?
You should consult a urologist if:
- Symptoms persist for more than 2 days
- You have a high fever, chills, or back pain
- UTIs occur frequently (more than 3 times a year)
- There is blood in your urine
- You are pregnant and experiencing UTI symptoms
- You have underlying conditions like diabetes or kidney disease
In such cases, seeing one of the Best Urologists in Dhaka can ensure proper diagnosis and treatment to avoid complications.
Diagnosis of Urine Infection
- Urine Test (Urinalysis): Detects white blood cells, red blood cells, and bacteria.
- Urine Culture: Identifies the specific bacteria causing the infection.
- Imaging Tests: Like ultrasound or CT scans (in recurrent or complicated cases).
- Cystoscopy: A procedure to examine the bladder and urethra, used in chronic cases.
Treatment Options
1. Antibiotics
- The first line of treatment.
- Course duration varies based on the severity of the infection.
- Always complete the full course as prescribed.
2. Pain Relief
- Over-the-counter pain relievers like ibuprofen or acetaminophen can help reduce discomfort.
3. Hydration
- Drink plenty of water to help flush out the bacteria.
4. Hospitalization
- Needed for severe infections, especially if they involve the kidneys or occur in immunocompromised individuals.
Preventing Urine Infections
- Drink at least 8 glasses of water daily.
- Urinate before and after sexual activity.
- Wipe front to back after using the toilet.
- Avoid using harsh soaps or feminine hygiene sprays.
- Don’t hold in urine for long periods.
- Wear cotton underwear and avoid tight-fitting clothes.
Final Thoughts
Urine infections can be painful, uncomfortable, and sometimes dangerous if left untreated. Recognizing the symptoms early and getting the appropriate treatment is the key to preventing serious complications. Whether you are experiencing a one-time infection or dealing with frequent UTIs, consulting a qualified urologist can make all the difference.
- Category : Blogpage
- 2025-06-01
- Views : 170
-
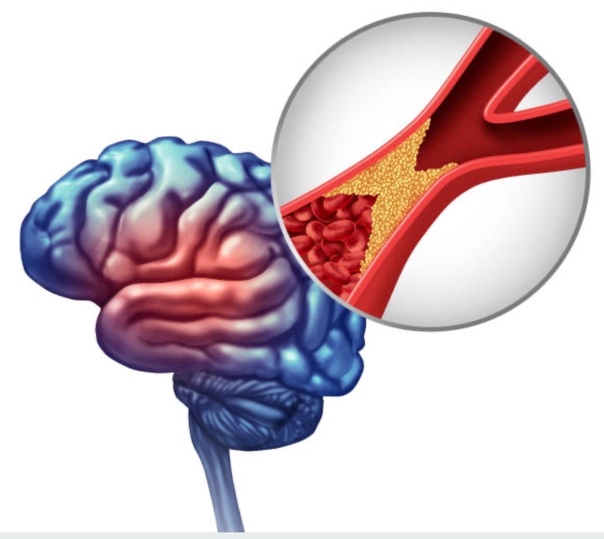
Brain Stroke Symptoms: Know the Warning Signs Before Its Too Late
A brain stroke is a medical emergency that occurs when blood flow to a part of the brain is interrupted or reduced. Without oxygen and nutrients, brain cells begin to die within minutes. Immediate treatment is crucial to minimize brain damage and improve outcomes. The best way to protect yourself and your loved ones is to understand the early symptoms of brain stroke, so you can act fast.
In this blog post, we will explore:
- What is a brain stroke?
- Different types of strokes
- Common brain stroke symptoms
- Why quick medical help is critical
- When to consult a neuromedicine specialist
What Is a Brain Stroke?
A brain stroke, also called a cerebrovascular accident (CVA), happens when there is a blockage (ischemic stroke) or bleeding (hemorrhagic stroke) in the brain. This leads to the death of brain cells, which can cause temporary or permanent disability, and even death in severe cases.
Types of Brain Strokes
There are two main types of brain strokes:
- Ischemic Stroke:
This is the most common type, accounting for about 80% of strokes. It occurs due to a blocked artery caused by a clot or plaque buildup. - Hemorrhagic Stroke:
This occurs when a blood vessel in the brain ruptures, leading to bleeding inside or around the brain. High blood pressure is a major risk factor. - Transient Ischemic Attack (TIA):
Also known as a “mini-stroke,” this is a temporary blockage that usually lasts a few minutes but is a serious warning sign of a future stroke.
Brain Stroke Symptoms: What to Watch For
Recognizing stroke symptoms early can save a life. The most common and recognizable symptoms include:
1. Sudden Numbness or Weakness
- Especially on one side of the body (face, arm, or leg)
- The person may not be able to lift one arm or smile evenly
2. Confusion and Trouble Speaking
- Slurred speech or difficulty understanding language
- The person might not be able to form sentences properly
3. Sudden Trouble Seeing
- Blurred or blackened vision in one or both eyes
- Sudden double vision may also occur
4. Difficulty Walking or Loss of Balance
- Dizziness, unsteady gait, or lack of coordination
- A feeling of spinning (vertigo) may also be present
5. Sudden Severe Headache
- Often described as the “worst headache of their life”
- May be accompanied by vomiting or altered consciousness
6. Facial Drooping
- One side of the face may droop or feel numb
- Ask the person to smile—if one side droops, it could be a stroke
FAST Test: Quick Way to Identify Stroke
Use the FAST test to quickly check for signs of stroke:
- F – Face: Ask the person to smile. Does one side of the face droop?
- A – Arms: Ask them to raise both arms. Does one arm drift downward?
- S – Speech: Ask them to repeat a simple sentence. Is the speech slurred?
- T – Time: If you notice any of these signs, call emergency services immediately.
Other Less Common Stroke Symptoms
- Sudden nausea or vomiting without a known cause
- Hiccups or difficulty breathing (more common in women)
- Sudden fatigue or altered mental state
- Seizures or loss of consciousness
Who Is at Risk?
Some people have a higher risk of stroke due to medical and lifestyle factors. These include:
- High blood pressure (Hypertension)
- Diabetes
- High cholesterol
- Heart disease
- Smoking and alcohol abuse
- Obesity and physical inactivity
- Family history of stroke
- Older age (above 55)
Importance of Early Diagnosis and Treatment
Brain stroke is a time-sensitive medical condition. The sooner the treatment begins, the better the chances of recovery. Treatments like thrombolytic therapy (for ischemic stroke) can dissolve clots if given within a few hours of symptom onset.
Delaying treatment can lead to:
- Permanent disability
- Memory loss
- Speech and language difficulties
- Paralysis or motor weakness
- Risk of recurrent stroke
- Death in severe cases
That’s why it's important to consult a qualified neuromedicine specialist in Dhaka if you or someone you know is experiencing stroke symptoms or is at risk due to existing health conditions.
What a Neuromedicine Specialist Can Do
A neuromedicine specialist focuses on diagnosing and treating disorders related to the brain, spinal cord, and nervous system. For stroke patients, they:
- Conduct detailed neurological examinations
- Recommend brain imaging (MRI/CT Scan)
- Prescribe appropriate medications
- Develop rehabilitation plans (physiotherapy, speech therapy)
- Provide long-term care and stroke prevention strategies
Final Thoughts
A brain stroke can change a person’s life within minutes—but timely recognition and immediate medical care can make a huge difference. By understanding the early symptoms of brain stroke and acting fast, you can help prevent permanent damage or even save a life.
- Category : Doctors
- 2025-06-01
- Views : 142
-
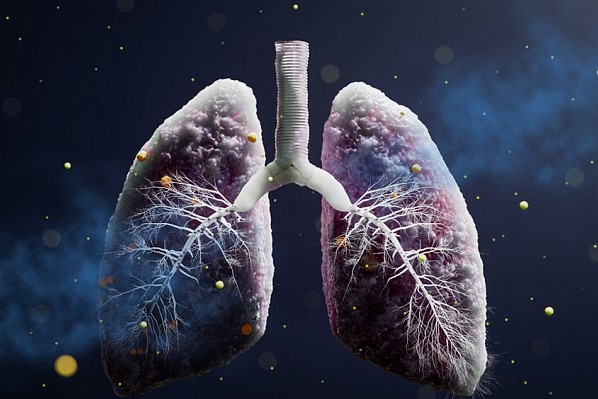
Lung Infection Symptoms: What You Need to Know
Lung infections are a common but serious health condition that can affect people of all ages. They can range from mild respiratory issues to life-threatening conditions like pneumonia. Recognizing the symptoms early can help you seek timely medical attention and avoid serious complications.
In this blog post, we’ll explore the symptoms of lung infections, the different types, when to seek medical help, and why it's essential to consult a Chest Specialist if you're experiencing respiratory problems.
What is a Lung Infection?
A lung infection occurs when viruses, bacteria, or fungi invade the lungs and cause inflammation. The most common types of lung infections include:
- Pneumonia – an infection that inflames the air sacs in one or both lungs
- Bronchitis – inflammation of the bronchial tubes
- Tuberculosis (TB) – a serious bacterial infection caused by Mycobacterium tuberculosis
- COVID-19 – a viral infection affecting the respiratory system
- Fungal infections – like aspergillosis, more common in people with weakened immune systems
Each of these infections presents with slightly different symptoms, but many overlap.
Common Lung Infection Symptoms
Recognizing the symptoms of a lung infection is crucial for early diagnosis and treatment. Below are the most common signs to watch out for:
1. Persistent Cough
A cough that lasts for more than a week could indicate a lung infection. It may start dry and become productive, producing mucus or phlegm.
- Color of mucus may vary from clear to yellow, green, or even blood-streaked.
- A worsening cough, especially with chest pain, should not be ignored.
2. Shortness of Breath
Breathlessness is a common symptom of more severe lung infections like pneumonia or COVID-19.
- You may feel winded after minimal activity.
- In extreme cases, it may feel difficult to breathe even while resting.
3. Chest Pain
Infections can cause inflammation in the lungs and pleura (the lining around the lungs), leading to chest discomfort.
- The pain may worsen with deep breaths or coughing.
- It might feel like a sharp or stabbing sensation.
4. Fever and Chills
A high temperature is your body’s way of fighting off infection. Lung infections, particularly bacterial ones, often cause:
- Fever above 100.4°F (38°C)
- Chills and sweating episodes
- Night sweats in conditions like TB
5. Fatigue and Weakness
Fighting an infection consumes a lot of energy, leaving you feeling drained or weak. Fatigue can be mild or severe depending on the type and severity of the infection.
6. Wheezing or Noisy Breathing
A wheezing or crackling sound while breathing is common in people with lung infections. It indicates restricted airways or fluid in the lungs.
- Listen for a high-pitched whistling sound during exhalation.
7. Bluish Lips or Fingertips
This condition, known as cyanosis, is a sign that oxygen levels in your blood are dangerously low.
- It requires immediate medical attention.
8. Loss of Appetite and Nausea
Lung infections can disrupt your appetite and cause gastrointestinal symptoms like nausea, especially if the infection is viral.
Symptoms in Different Age Groups
- Children may present with rapid breathing, nasal flaring, or refusal to eat.
- Elderly patients might show confusion, weakness, and lower-than-normal body temperatures instead of a high fever.
When to See a Doctor
You should seek medical attention if:
- Symptoms persist for more than a week
- You experience high fever and chills
- Breathing becomes difficult
- Chest pain worsens
- You cough up blood
- Fatigue becomes debilitating
If you’re living in Dhaka or the surrounding areas, it’s advisable to consult a Chest Specialist in Dhaka for a proper diagnosis and treatment plan. These experts can perform necessary tests, such as chest X-rays, CT scans, and sputum analysis, to determine the cause of the infection and recommend appropriate antibiotics or antivirals.
Diagnosis and Treatment
Diagnosis:
- Physical exam and review of symptoms
- Imaging tests like chest X-ray or CT scan
- Lab tests such as blood work and sputum culture
- Pulse oximetry to measure oxygen levels
Treatment:
- Antibiotics for bacterial infections
- Antivirals for viral infections
- Antifungals for fungal infections
- Oxygen therapy for severe breathing issues
- Rest and fluids to help the body recover
Prevention Tips for Lung Infections
- Get vaccinated against flu, pneumonia, and COVID-19
- Practice good hygiene – wash hands frequently
- Avoid smoking and exposure to polluted air
- Strengthen your immune system with proper diet and exercise
- Wear a mask in crowded or dusty environments
- Manage chronic conditions like asthma or diabetes
Final Thoughts
Lung infections can range from mild to life-threatening. Being aware of the symptoms and acting early can significantly improve your chances of recovery. Whether it’s a lingering cough, chest pain, or breathing difficulty, never ignore the warning signs.
- Category : Blogpage
- 2025-05-29
- Views : 402
-
Causes of Chronic Kidney Disease (CKD): A Detailed Guide
Chronic Kidney Disease (CKD) is a progressive condition where the kidneys gradually lose their ability to function properly over time. The kidneys play a crucial role in filtering waste, balancing electrolytes, and regulating blood pressure. When this function is compromised, it can lead to serious health complications, including kidney failure, heart disease, and stroke.
Understanding the causes of chronic kidney disease is essential for early diagnosis, prevention, and treatment. In this article, we’ll explore the major causes of CKD and how you can protect your kidney health.
What is Chronic Kidney Disease?
Chronic Kidney Disease is defined as a gradual loss of kidney function over a period of months or years. It typically progresses in five stages, with Stage 1 being the mildest and Stage 5 indicating kidney failure that requires dialysis or a transplant.
Unlike acute kidney failure, CKD develops slowly and often shows no symptoms in its early stages. That’s why it's often called a “silent” disease.
Common Causes of Chronic Kidney Disease
Several factors can lead to the development of chronic kidney disease. Below are the most common causes:
1. Diabetes (Type 1 and Type 2)
Diabetes is the leading cause of chronic kidney disease. High blood sugar levels can damage the blood vessels in the kidneys, making it harder for them to filter waste and excess fluid.
- Diabetic nephropathy is a specific kidney condition caused by long-term diabetes.
- Managing blood sugar levels can significantly reduce the risk of CKD.
2. High Blood Pressure (Hypertension)
High blood pressure is the second most common cause of CKD. When blood pressure is consistently high, it puts stress on the tiny blood vessels in the kidneys.
- This pressure can cause the vessels to weaken or narrow, reducing kidney function.
- Controlling blood pressure through medication, diet, and lifestyle is essential for kidney health.
3. Glomerulonephritis
Glomerulonephritis is an inflammation of the kidney’s filtering units, called glomeruli. This condition can occur suddenly or develop over time.
- It may result from infections, autoimmune diseases, or unknown causes.
- Chronic glomerulonephritis is a significant contributor to CKD.
4. Polycystic Kidney Disease (PKD)
PKD is a genetic disorder that causes fluid-filled cysts to grow in the kidneys. Over time, these cysts can damage kidney tissue and impair function.
- It is one of the most common inherited kidney diseases.
- Symptoms often appear in adulthood and include high blood pressure, back pain, and kidney stones.
5. Obstruction of Urinary Tract
Blockages in the urinary tract can lead to a backup of urine, causing damage to the kidneys.
- Common causes include kidney stones, an enlarged prostate, or tumors.
- Prompt treatment of urinary obstructions is crucial to prevent CKD.
6. Repeated Kidney Infections (Pyelonephritis)
Frequent kidney infections can lead to scarring and damage that impair kidney function over time.
- Chronic infections often result from urinary tract abnormalities.
- Antibiotic treatment is necessary to control infections and prevent kidney damage.
7. Autoimmune Diseases
Diseases like lupus and IgA nephropathy can attack the kidneys directly or cause inflammation that damages kidney tissues.
- Early diagnosis and immunosuppressive therapy can help manage these conditions.
- Routine kidney function tests are recommended for individuals with autoimmune diseases.
8. Use of Certain Medications
Long-term use of certain drugs can be harmful to the kidneys.
- Pain relievers like NSAIDs (e.g., ibuprofen, naproxen), certain antibiotics, and contrast dyes used in imaging tests can contribute to CKD.
- Always consult a healthcare provider before taking medications for extended periods.
9. Toxins and Environmental Factors
Exposure to heavy metals (like lead or mercury), industrial chemicals, or contaminated water can increase the risk of kidney disease.
- Occupational safety measures and avoiding unregulated herbal remedies are essential precautions.
10. Family History of Kidney Disease
Having a close family member with kidney disease increases your risk. While genetics play a role, shared lifestyle factors and early screening can help manage this risk.
Symptoms of Chronic Kidney Disease
In the early stages, CKD often shows no symptoms. As it progresses, common symptoms include:
- Fatigue and weakness
- Swelling in the feet and ankles
- Changes in urination
- Shortness of breath
- High blood pressure
- Persistent itching
If you experience any of these symptoms, consult a Kidney Specialist Doctor for proper evaluation and diagnosis.
Prevention Tips for Chronic Kidney Disease
While not all causes of CKD are preventable, you can take the following steps to reduce your risk:
- Manage diabetes and blood pressure effectively
- Maintain a healthy diet low in sodium and protein
- Avoid smoking and excessive alcohol consumption
- Exercise regularly
- Get regular checkups, especially if you have a family history of kidney disease
- Stay hydrated, but don’t overdo it
- Avoid over-the-counter medications that can harm your kidneys
Final Thoughts
Chronic kidney disease is a serious condition that often goes unnoticed until it's advanced. Understanding its causes—from diabetes and hypertension to genetic disorders and infections—can help you take proactive steps to protect your kidney health. Early intervention is key to slowing the progression of the disease and maintaining a good quality of life.
- Category : Blogpage
- 2025-05-29
- Views : 84
-
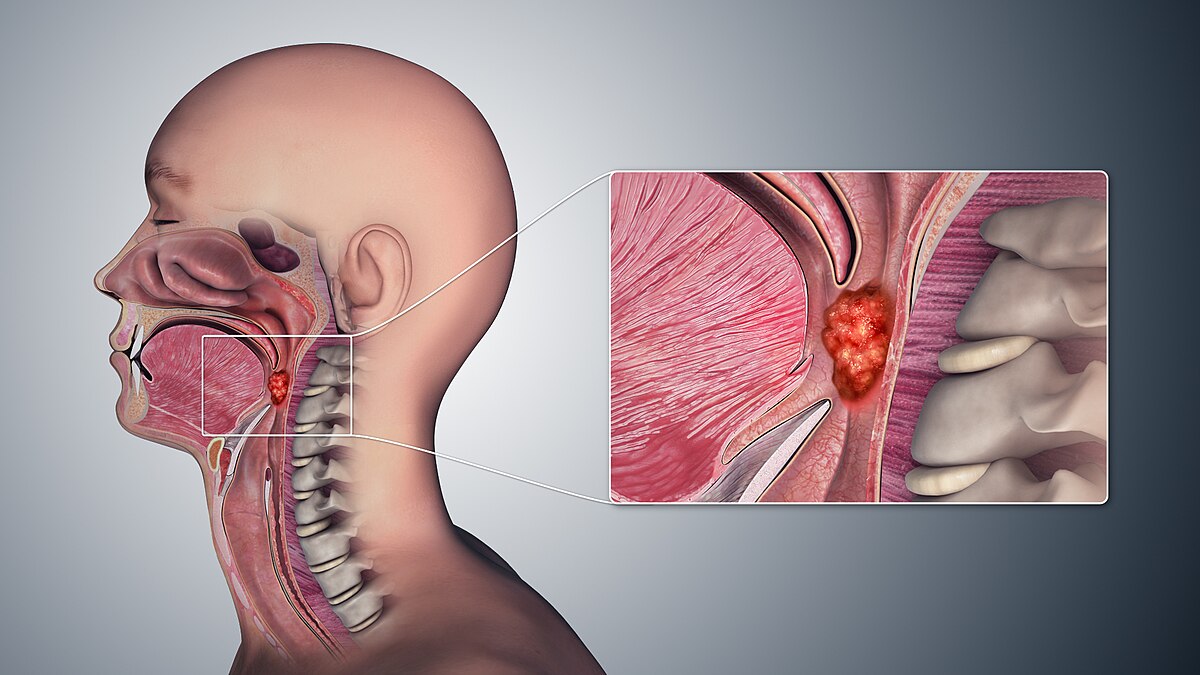
Throat Cancer Symptoms: Early Signs You Should Never Ignore
Throat cancer, although not as common as some other cancers, is a serious and potentially life-threatening condition that affects thousands of people worldwide every year. In Bangladesh, cases are increasing, particularly due to lifestyle habits such as smoking, tobacco chewing, and poor oral hygiene. Detecting throat cancer symptoms early can greatly improve treatment outcomes and survival rates.
In this blog post, we’ll discuss what throat cancer is, highlight its most common and uncommon symptoms, explore risk factors, and explain when to see a specialist.
What is Throat Cancer?
Throat cancer refers to cancerous tumors that develop in your throat (pharynx), voice box (larynx), or tonsils. It is a type of head and neck cancer. The most common types include:
- Pharyngeal cancer – affects the throat behind the nose and mouth.
- Laryngeal cancer – involves the voice box.
- Tonsil cancer – affects the tonsils at the back of the throat.
Common Throat Cancer Symptoms
The early symptoms of throat cancer can mimic those of a common cold, making them easy to overlook. However, persistent or unusual symptoms should never be ignored.
1. Persistent Sore Throat
A sore throat that doesn’t go away even after a few weeks and doesn’t respond to typical treatment (like antibiotics) could be a sign of throat cancer.
2. Hoarseness or Voice Changes
A raspy or hoarse voice lasting more than two weeks is one of the earliest signs, especially in cancers of the larynx.
3. Difficulty Swallowing (Dysphagia)
Throat cancer can make swallowing painful or cause the sensation that food is stuck in your throat.
4. Lump in the Neck
Swollen lymph nodes or a lump in the neck that persists may indicate cancer spreading from the throat to nearby tissues.
5. Unexplained Weight Loss
Sudden, unexplained weight loss can be a general sign of cancer, including throat cancer.
6. Chronic Cough or Coughing Up Blood
A nagging cough or blood in your saliva/phlegm should be investigated immediately.
Other Symptoms You Should Know
- Ear pain without an ear infection
- Bad breath that doesn’t go away
- Fatigue or general weakness
- Difficulty opening the mouth or moving the tongue
- Noisy breathing or wheezing
Throat Cancer in Early vs Late Stages
Early-stage symptoms are usually mild but persistent:
- Hoarseness
- Slight discomfort while swallowing
- Mild sore throat
Late-stage symptoms can be severe:
- Complete voice loss
- Inability to swallow
- Severe pain
- Noticeable lump in the throat or neck
- Significant weight loss
Major Risk Factors
Understanding the risk factors can help you take preventive action:
- Smoking and tobacco use
- Alcohol abuse
- HPV (Human Papillomavirus) infection
- Poor oral hygiene
- Exposure to certain chemicals
- Gastroesophageal reflux disease (GERD)
Men are more likely than women to develop throat cancer, and the risk increases with age.
When to See a Doctor?
If you experience any of the above symptoms for more than two weeks, it is essential to consult an ENT (Ear, Nose, and Throat) specialist. Early detection through a simple throat examination, biopsy, or imaging can make a huge difference in your treatment success.
Looking for expert care? It’s important to find the best ENT specialist for accurate diagnosis, biopsy, endoscopic evaluation, and comprehensive treatment plans. Specialists can detect whether your symptoms are benign or something more serious like cancer.
Diagnosis and Tests
After an initial examination, your ENT specialist may recommend:
- Laryngoscopy or Endoscopy – to view the inside of the throat.
- Biopsy – to examine tissue under a microscope.
- CT Scan, MRI, or PET Scan – to detect cancer spread.
- HPV Testing – especially for oropharyngeal cancer.
Treatment Options
Treatment depends on the cancer stage and location:
- Surgery – to remove tumors in early stages.
- Radiation Therapy – often used for small or localized tumors.
- Chemotherapy – for advanced cancer or in combination with radiation.
- Targeted Therapy – drugs that block the growth of cancer cells.
- Rehabilitation – including speech therapy if the voice box is affected.
Preventing Throat Cancer
While not all cases are preventable, the following steps can greatly reduce your risk:
- Quit smoking and avoid tobacco in all forms.
- Limit or avoid alcohol consumption.
- Get vaccinated against HPV.
- Maintain good oral hygiene.
- Eat a diet rich in fruits and vegetables.
- Avoid exposure to carcinogenic chemicals.
- Treat acid reflux promptly.
Final Words
Throat cancer is a serious condition, but early detection significantly boosts the chances of successful treatment. If you’ve had a sore throat, hoarseness, or trouble swallowing for more than two weeks, don’t wait—get evaluated by an ENT specialist.
Remember, early diagnosis can save lives. For proper assessment, diagnosis, and treatment of persistent throat symptoms, it’s crucial to consult an ENT Specialist.
- Category : Blogpage
- 2025-05-28
- Views : 1178
Popular posts
ঢাকার চর্ম রোগ বিশেষজ্ঞ সেরা ১০ ডাক্তার তালিকা।
- Category : Doctors
- 2023-11-29
- Views : 66375
ঢাকার চর্ম রোগ বিশেষজ্ঞ সেরা ১০ ডাক্তার তালিকা।

ঢাকার সেরা ১০ নিউরোলজি বিশেষজ্ঞ ডাক্তারদের তালিকা
- Category : Doctors
- 2025-04-29
- Views : 65161
ঢাকার সেরা ১০ নিউরোলজি বিশেষজ্ঞ ডাক্তারদের তালিকা

ঢাকার চর্ম ও যৌন রোগ বিশেষজ্ঞ ডাক্তারের তালিকা
- Category : Doctors
- 2022-09-18
- Views : 54597
ঢাকার চর্ম ও যৌন রোগ বিশেষজ্ঞ ডাক্তারের তালিকা











